What Is Claim Processing in Health Insurance (2022) ?
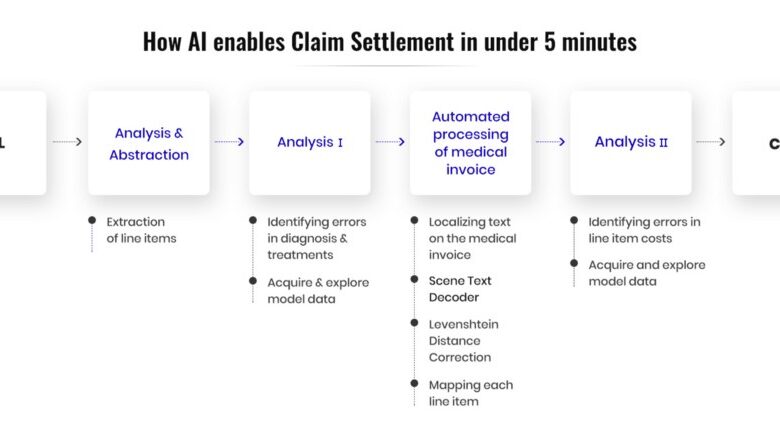
There are several steps involved in health insurance claim processing. If you have an insurance policy, you should be aware of the types of services that are covered and the network of doctors that participate in your plan. Once you have made an appointment, the process will begin almost immediately. You’ll go through a series of steps to receive your final bill. Once you’ve been treated, your claim will be processed for reimbursement. Fortunately, there are a few things you can do to expedite the process.
First, verify your eligibility. Many insurance companies offer a cashless claim process that allows you to submit your claim online. The first step is to verify that you have the correct insurance. This step involves verifying that you have received a medical bill. After you’ve verified the validity of a patient, you’ll need to process the claim. Using an online tool is a great way to streamline this task.
Once you’ve completed the form, you’ll need to submit it to the insurance company. After it is processed, the insurance company will evaluate it and settle the amount owed by the healthcare provider. Depending on the type of claim, the process may be a simple reimbursement process or a complex cashless claim process. You can find the right form for your specific plan by logging in to the website of your health insurance provider.
The process also helps the insurer to make payments. In addition to reviewing the medical data, medical claims processing reviews and approves claims. The process helps the insurance provider fulfill its commitment to its customers. In turn, it helps the company deliver on its promises. For this reason, it’s an integral part of the health insurance business. It allows you to receive the compensation that you’re due. You’ll never have to worry about getting paid again.
When you have a medical emergency, you’ll need to file a claim. You’ll need to provide the necessary information, which will allow the insurance company to process your claim. You’ll need to include details of your condition. A medical claim processing company will ensure that you’re compliant with all rules and regulations. The process ensures that your health insurance company pays the right amount for your medical care.
The claims processor is responsible for evaluating the medical bills sent by medical providers. The process involves preparing the claims. The claim is then checked for completeness and accuracy and is then submitted to the insurance company. After a claim is processed, the insurance company will pay the healthcare provider. Then, the claim will be processed. The insurance company will review the information and determine if it is covered by your plan. There are several steps to claim processing.
Once your claim has been approved, the insurance company will process it. In most cases, the claims are processed manually. However, you can choose to submit them electronically. Using a third-party administrator can save you $3 per claim. By following the steps in the claims processing process, you’ll get the right payment for your medical care. It also saves the insurance company time. In the end, the insurance company will settle the claims and pay out the money to the healthcare provider.
Once you’ve filed a claim, the insurance company will verify that it is valid. Then, the claims will be processed for payment. The entire process takes place at a single location. For example, a doctor’s office will send the claim to a third-party administrator. The insurance company will send it to a claims processing department. The process will take a few weeks to complete. After the claims are processed, the insurer will pay out the remaining amount.
The process of claim processing in health insurance starts with the physician’s office. This office will gather the relevant information from the insurance form, medical codes, and other relevant information. The claim will then be sent to a claims processing department or a third-party administrator. After a few weeks, the patient will get a bill for the remaining cost. The claim forms will need to be filed electronically and can be found in the health insurance company’s website.




